Study of two million people: Inherited risk for mental illness spills across diagnostic lines far more than realized
Massive Swedish study of over two million people reveals that genetic risk for mental illness often points toward multiple disorders, not just the one diagnosed
Genetic specificity is not some abstract property locked inside the genome. We have been debating whether psychiatric disorders are truly distinct since the 1800s. Now we can put numbers on it.”
RICHMOND, VA, UNITED STATES, March 3, 2026 /EINPresswire.com/ -- There is a question that has haunted psychiatry since before it had a name, back when the alienists in their frock coats were still debating whether madness ran in families or simply accumulated there like dust. The question is deceptively simple. When a person inherits a vulnerability to mental illness, does that vulnerability have an address? Does it point, with any precision, toward the specific disorder that eventually appears on the chart? Or does it scatter, landing across the whole landscape of the mind like seed thrown from a moving hand?— Dr. Kenneth S. Kendler, Virginia Commonwealth University
A sweeping new study published in Genomic Psychiatry has, for the first time, put actual numbers on the answer. The numbers are not what most clinicians expected.
Dr. Kenneth S. Kendler, a psychiatric geneticist at Virginia Commonwealth University, led a team that analyzed data from more than two million individuals born in Sweden between 1950 and 1995. The dataset drew from national patient registries and primary care records covering essentially the entire population. The team selected nine major psychiatric and substance use disorders: schizophrenia, bipolar disorder, major depression, anxiety disorder, PTSD, ADHD, autism spectrum disorder, alcohol use disorder, and drug use disorder. For each one, they calculated a measure they call genetic specificity: the percentage of total inherited risk in a person with a given diagnosis that actually points toward that diagnosis and not toward the others.
Think of it this way. If you have been diagnosed with depression, some of your genetic risk factors genuinely predispose you to depression. But some of them, possibly most of them, actually predispose you to anxiety, or substance use problems, or ADHD, or conditions your doctor never mentioned. Genetic specificity tells you what fraction of the total genetic signal is truly about the diagnosis on your chart.
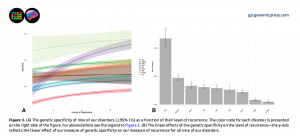
The results arranged themselves into a hierarchy that nobody had previously quantified, and it was stark. Schizophrenia sat at the top with a genetic specificity of 73.1%, meaning nearly three quarters of the aggregate genetic risk carried by individuals with schizophrenia coded exclusively for schizophrenia. Whatever else it may be, schizophrenia is, genetically speaking, overwhelmingly its own thing. Bipolar disorder followed at 54.8%. Alcohol use disorder came in at 54.1%.
A middle tier held some surprises. ADHD registered 48.2%, autism spectrum disorder 47.5%, and PTSD 47.4%. Three conditions that look nothing alike in a clinic waiting room turned out to occupy nearly identical genetic ground.
Then came the conditions whose genetic identities were the most blurred. Major depression landed at 41.1%. Anxiety disorder at 38.6%. And drug use disorder, at the bottom of the list, registered a mere 29.5%. That last number deserves a pause. It means that for every unit of genetic risk carried by someone diagnosed with drug use disorder, less than a third of it is actually about drugs. The remaining two thirds scatter across schizophrenia, depression, ADHD, and the other conditions in the panel. The genes do not know what the clinician wrote on the form.
"What surprised us was the sheer range," said Dr. Kenneth S. Kendler, VIPBG Distinguished Professor of Psychiatry at Virginia Commonwealth University and corresponding author of the study. "Schizophrenia carries a genetic signature that is overwhelmingly its own. Drug use disorder, by contrast, looks more like a downstream expression of genetic risks that cut across many conditions. That difference has real implications for how we design genetic studies and how we think about diagnostic categories."
Could this finding reshape how doctors think about the boundaries between one mental illness and another? Could it mean that some of the categories clinicians spend entire careers distinguishing are, at the genetic level, less distinct than anyone assumed? The data strongly suggest yes.
But the most provocative finding may be this: genetic specificity is not fixed. It moves. It shifts, sometimes dramatically, depending on three features that any clinician can observe. Age at onset. Number of recurrent episodes. And where the patient receives treatment.
Bipolar disorder showed the widest swings. Patients whose illness began early in life had substantially higher genetic specificity than those with late onset, and the drop-off was steep. Patients with many recurrent episodes were far more genetically specific than those with few. And here is where it gets clinically fascinating: bipolar patients treated in hospitals carried a genetic specificity of 63%, while those seen only in primary care registered just 31%, a gap of more than thirty percentage points (p < 0.001). What lands a bipolar patient in a hospital bed is typically the severity of the manic episode itself, which concentrates the disorder-specific genetic signal. Primary care bipolar, by contrast, may represent a milder, more genetically diffuse presentation.
PTSD moved in the opposite direction. Its genetic specificity actually increased with later age at onset and was highest among individuals treated only in primary care, at 53%, compared with 41% for those who were hospitalized. The reasons likely differ: hospitalized PTSD may involve more comorbid conditions that dilute the disorder-specific signal.
For all nine disorders without exception, greater recurrence was associated with higher genetic specificity. The effect was most pronounced for bipolar disorder and ADHD. The logic is intuitive once you see it: a person who keeps returning to the same illness, episode after episode, year after year, probably carries genes that are genuinely aimed at that illness, rather than a generalized vulnerability that happened to land there once by circumstance.
What does this mean for the family doctor in a small town who sees a forty-five-year-old patient walk in with a first episode of depression? Is that patient genetically the same as a twenty-year-old with recurrent depression? The data say no. And the difference is not subtle.
"Genetic specificity is not some abstract property locked inside the genome," Dr. Kendler explained. "It moves. It responds to clinical features that every psychiatrist can observe at the bedside. A hospitalized bipolar patient and one seen only in primary care carry substantially different levels of genetic specificity."
One of the most intellectually satisfying puzzles in the study involves the contrasting behavior of depression and bipolar disorder at the hospital door. For bipolar disorder, hospitalization concentrates the genetic signal. It makes sense: the manic episode is what drives the admission, and mania is the core of the disorder. But for depression, hospitalization does the opposite. Hospitalized depression cases were less genetically specific than those treated in primary care. The researchers propose a reason that will resonate with anyone who has worked in an emergency room: what brings a depressed person to the hospital is often not the depth of the sadness itself but impulsive behavior, suicidal crises, and substance-related emergencies, all of which reflect elevated genetic risk for externalizing disorders like ADHD and substance use. The depression you see in primary care, the quieter kind, may carry a purer genetic signal for mood pathology.
The question practically asks itself. Should researchers studying the genetics of depression be recruiting from family medicine clinics rather than inpatient psychiatric units? Would that produce cleaner, more replicable genetic findings? The authors do not say so explicitly, but the data lean hard in that direction.
The investigators stress-tested their findings with the care of engineers checking a bridge. Sensitivity analyses explored what happened when they removed patients who carried more than one diagnosis. Stripping out the 6.0% of depression cases who also had a lifetime bipolar diagnosis barely moved the specificity estimate, from 41.1% to 41.8%. Similar corrections for the overlap between schizophrenia and bipolar disorder produced equally small shifts. The hierarchy held.
Sex-stratified analyses showed that genetic specificities were remarkably similar between men and women for most conditions. The two clear exceptions were alcohol use disorder and drug use disorder, where men showed substantially higher genetic specificities (p < 0.001). Whether this reflects biological differences or the possibility that social and environmental factors dilute disorder-specific genetic signals differently in women remains an open and important question.
The results converge compellingly with recent molecular genetics. A large multivariate study by Grotzinger and colleagues, published in Nature in 2026, examined fourteen psychiatric disorders using polygenic risk scores and identified a general psychopathology factor, a kind of master dial for mental illness liability. Their internalizing factor, which included major depression, anxiety disorder, and PTSD, the three conditions with the lowest genetic specificity in Dr. Kendler's analysis, shared more than 90% of its genetic variance with that general factor. The schizophrenia-bipolar factor shared only 35%. Two entirely different research groups, using entirely different methods and different populations, arrived at the same conclusion: some psychiatric disorders have sharp genetic borders, and some do not.
The study carries honest limitations. It relies on Swedish national registry data, not structured diagnostic interviews conducted by researchers. Diagnostic practices vary across clinicians and eras. The population studied was Swedish-born individuals from Swedish-born parents, and whether the same hierarchy would appear in other ethnic and geographic populations remains unknown. The family genetic risk scores used here differ fundamentally from the polygenic risk scores derived from DNA sequencing, although the Kendler team has previously shown that the two approaches behave consistently.
There is also a deeper structural point worth noting. Genetic specificity is partly shaped by comorbidity. A disorder that is only moderately heritable and that frequently co-occurs with other conditions, as depression does with anxiety and substance use, will almost inevitably show lower specificity. A highly heritable disorder with relatively little comorbidity, like schizophrenia, will show high specificity. Both predictions are borne out in the data. This does not diminish the findings. It places them in context.
Could replication in non-Scandinavian cohorts reveal different hierarchies? Might populations with different genetic architectures or healthcare systems produce different patterns? These remain open questions of real significance.
"We have been debating whether psychiatric disorders are truly distinct since the 1800s," Dr. Kendler reflected. "Now we can actually put numbers on it. Some of our diagnostic categories carve nature much more cleanly at the genetic joints than others, and clinicians and researchers alike need to reckon with that."
If genetic specificity varies predictably with observable clinical features, then researchers designing genetic studies could begin selecting participants to sharpen or broaden the signal, depending on what they are trying to find. Clinicians might someday use specificity-related markers, age at onset, recurrence patterns, treatment history, to refine prognosis and guide treatment. And the nosologists, the scientists who build the diagnostic manuals that every doctor in the country consults, now have a quantitative framework for asking the most uncomfortable question in their field: how genetically real are the categories we have been using?
The sample sizes were formidable. The depression cohort alone included 674,955 individuals. Schizophrenia comprised 18,348. The total dataset encompassed more than two million diagnostic records with full population coverage.
This peer-reviewed research represents a significant advance in psychiatric genetics, offering new insights into the genetic architecture of mental illness through rigorous population-based investigation. The findings challenge existing assumptions about diagnostic boundaries by demonstrating that genetic specificity varies widely across disorders and is modifiable by clinical features. By employing family genetic risk scores calculated from national Swedish registries encompassing over two million affected individuals, the research team has generated data that not only advances fundamental knowledge but suggests practical applications in genetic study design and clinical stratification. The interdisciplinary collaboration between psychiatric genetics at Virginia Commonwealth University and primary care epidemiology at Lund University demonstrates the power of combining diverse expertise to tackle complex scientific questions.
This project was supported in part by NIH grants R01DA030005, R01MH139865 and R01AA023534 and the Swedish Research Council (2024-02796 and 2021-06467).
The Research Article in Genomic Psychiatry titled "The specificity of genetic risk for psychiatric and substance use disorders: Its modification by age at onset, recurrence, and site of treatment" is freely available via Open Access on 3 March 2026 in Genomic Psychiatry at the following hyperlink: https://doi.org/10.61373/gp026a.0024.
About Genomic Psychiatry: Genomic Psychiatry: Advancing Science from Genes to Society (ISSN: 2997-2388, online and 2997-254X, print) represents a paradigm shift in genetics journals by interweaving advances in genomics and genetics with progress in all other areas of contemporary psychiatry. Genomic Psychiatry publishes medical research articles of the highest quality from any area within the continuum that goes from genes and molecules to neuroscience, clinical psychiatry, and public health.
Visit the Genomic Press Virtual Library: https://issues.genomicpress.com/bookcase/gtvov/
Our full website is at: https://genomicpress.com/
Ma-Li Wong
Genomic Press
mali.wong@genomicpress.com
Legal Disclaimer:
EIN Presswire provides this news content "as is" without warranty of any kind. We do not accept any responsibility or liability for the accuracy, content, images, videos, licenses, completeness, legality, or reliability of the information contained in this article. If you have any complaints or copyright issues related to this article, kindly contact the author above.